Bionic limbs
Expert reviewers
Essentials
- Bionics can be highly advanced pieces of technology, able to be integrated with various parts of the human body.
- Bionic limbs are constantly evolving and becoming more lifelike in their form and function.
- There are many different types of bionic limb technology available, each with its own benefits and drawbacks.
- Bionic limbs still have a long way to go before they achieve the full range of motion, control and sensitivity of ‘biological’ limbs.
Faster? Stronger? More powerful? Bionic bodies—and what they may be capable of—have captivated the human mind for centuries. From the bumbling Inspector Gadget to the near‐indestructible Terminator, the idea of using technology to build a ‘better human’ has resulted in continuous technological advances.
The term ‘bionics’ was first used in the 1960s. It combines the prefix ‘bio’—meaning life—with the ‘nics’ of electronics. Bionics is the study of mechanical systems that function like living organisms or parts of living organisms.
Artificial limbs, or prostheses, are used to replace a missing body part which may have been lost due to trauma, disease or congenital defect. The type of prosthesis a person can use is dependent on the individual, including the cause of amputation or limb loss, and the location of the missing extremity.
Basic artificial limbs have been used since 600 BC. Wooden legs, metal arms, hooks for hands—while these primitive replacements gave the wearer back some semblance of movement or function, they were often uncomfortable, difficult to use, had poor functionality and were cosmetically unattractive.

Today, researchers are striving to develop lighter, smaller, better‐controlled, more lifelike and affordable options. What’s different about the new generation of prosthetic limbs is their union with bionic technology, and the way they combine fields of study as diverse as electronics, biotechnology, hydraulics, computing, medicine, nanotechnology and prosthetics. Technically, the field is known as biomechatronics, an applied interdisciplinary science that works to integrate mechanical elements and devices with biological organisms such as human muscles, bones, and the nervous systems.
External prosthetic limbs
Recent progress in both materials science and technology has resulted in significant advancements in prosthetic limbs. While it’s tempting to imagine these limbs as giving the wearer some kind of superhuman edge, in reality, researchers at present are simply trying to recreate the functionality and range of motion experienced by a healthy human limb. This is more difficult than it sounds.
Think about it—if your nose is itchy, you scratch it. But take a moment to consider how you actually do this. First, you need to bend your elbow while raising your forearm so that it’s in the correct position close to your nose. Then you need to rotate your forearm to the required angle so that your finger can reach your nose, then extend a finger and move it up and down repeatedly on the itch. And you have to do all this while applying the right amount of pressure to stop the itch, but without scratching off any skin. As you can imagine, creating a robotic limb to do all these things seamlessly, easily and quickly is quite a challenge.

So while giving a high five or walking up a flight of stairs might not seem like very complex activities, behind the scenes (or inside your head) your brain is constantly working to help you perform even the simplest gestures. Nerves, muscles, synapses, brain cortices—they all need to be working seamlessly to allow you to perform these tasks.
It is this interaction between thought, action and response that researchers across the world have been trying to replicate in their bionic technologies.
A number of bionic prosthetic limbs are now available which are beginning to mimic some of the functionality of the original lost limbs. Others are still at the research and development stage, but are showing great promise. Let’s take a look at some of them.
Myoelectric limbs
Traditionally, upper‐limb prostheses were body powered, using cables and harnesses attached to the individual and relying on body movements to manipulate cables that control the prosthetic limb. This can be physically tiring, cumbersome and unnatural.
Myoelectric limbs are externally powered, using a battery and electronic system to control movement. Each prosthesis is custom made, attaching to the residual limb using suction technology.
Once the device has been securely attached, it uses electronic sensors to detect even the smallest traces of muscle, nerve and electrical activity in the remaining limb. This muscle activity is transmitted to the surface of the skin where it is amplified and sent to microprocessors, which use the information to control the movements of the artificial limb.
Based on the mental and physical stimulus provided by the user, the limb moves and acts much like a natural appendage. By varying the intensity of the movement of their existing functional muscles the user can control aspects such as strength, speed and grip in the bionic limb. If muscle signals cannot be used to control the prosthesis, switches with a rocker, pull-push or touch pad can be used. Improved dexterity is achieved via the addition of sensors and motorised controls, thus enabling users to perform tasks such as using a key to open a door or getting cards out of a wallet.
One of the features of this technology is the ‘autograsp’ function, which automatically adjusts tension when it detects a change in circumstance (such as holding a glass that is then filled with water). An added bonus of the myoelectric limb is that, like traditional body-powered devices, it can be made to replicate the appearance of a natural limb.
The disadvantages of this technology are that the battery and motor inside it makes it heavy, it’s expensive, and there’s a slight time delay between the user sending a command and the computer processing that command and turning it into action.
Osseointegration
Another bionic limb breakthrough is known as ‘osseointegration’ (OI). Derived from the Greek ‘osteon’, meaning bone, and the Latin ‘integrare’, which means to make whole, the process involves creating direct contact between living bone and the surface of a synthetic—often titanium‐based—implant.
The procedure was first performed in 1994, and uses a skeletally integrated titanium implant, connected through an opening (stoma) in the residual limb to an external prosthetic limb. The direct connection between the prosthesis and bone has several advantages:
- It provides greater stability and control, and can reduce the amount of energy expended.
- It does not require suction for suspension, which makes it easier and more comfortable for the user.
- The weight‐bearing is brought back to the femur, hip joint, tibia or other bone, reducing the possibility of degeneration and atrophy that can accompany traditional prostheses.
Traditionally, the procedure requires two operations. The first involves the insertion of titanium implants into the bone and, often, extensive soft-tissue revision. The second stage, around six to eight weeks later, includes the refinement of the stoma and the attachment of the hardware that connects the implant to the external prosthetic leg. Gradually, bone and muscle begin to grow around the implanted titanium on the bone end, creating a functional bionic leg. The external prosthesis can be easily attached and removed from the abutment GLOSSARY abutmentthe portion of an implant that protrudes through the tissues and is designed to support a prosthesis. within a few seconds. Recently, Australia‐based surgeon Associate Professor Munjed Al Muderis has been able to perform the surgery in a single operation.
Because the prosthesis is attached directly to the bone, it has a greater range of movement, control and, in some cases, has allowed wearers to distinguish tactile difference between surfaces (such as carpet versus tiles) via osseoperception.

Gait-training, strengthening and rehabilitation are all important parts of the pre and post‐surgery procedure. Many of the recipients of the new technology have been up and walking independently within weeks of the operation, and have been able to regain much of their quality of life.
A continuing development in the field of OI is the introduction of products that use a porous metal construction, such as titanium foam. Traditional OI designs intended for the femur were not successful when applied to the tibia as the proximal tibial bone structure is highly spongy.However, with the development of titanium foam technology the application of OI has now been expanded to transtibial amputees. Associate Professor Al Muderis has pioneered a 3D-printed foam surface implant which is successfully used in transtibial amputees. These 3D-printed metal foams may promote and contribute to bone infiltration and the formation and growth of vascular systems within the defined area. In this way, the porous, bone‐like metal foam allows osteoblast GLOSSARY osteoblasta cell which secretes the substance of bone. activity to begin.
Recipients of the OI procedure say that it almost feels like the real thing. Drawbacks of this type of prosthesis are that it is costly (generally over A$80,000), and unsuitable for many types of amputee.
Mind‐controlled bionic limbs
The next advance in bionic limb technology is the emergence of mind‐controlled bionic limbs. These are prostheses which can be integrated with body tissues, including the nervous system. They are highly advanced, able to respond to commands from the central nervous system and therefore to more closely replicate normal movement and functionality, while also instantly triggering the desired movement with less ‘lag time’. There are several different procedures and technologies currently in the research and development phase.

Targeted muscle reinnervation
A surgery called targeted muscle reinnervation uses nerves remaining after an amputation, and the same impulses from the brain that once controlled flesh and blood, to control an artificial limb. The surgery reattaches nerves that control the joints from the missing part of the limb into muscle tissue in the residual limb to allow a more natural thought process and control the prosthesis the same way as myo-electric control. Effectively, the brain impulses are linked to a computer in the prosthesis that directs motors to move the limb.
In 2014, Les Baugh, a bilateral shoulder disarticulation (through the joint) amputee, was able to use this technology to operate two upper limb prosthesis for the first time. Working with researchers at Johns Hopkins University, he was able to lift cups and perform a variety of tasks with each arm, a result of a procedure which could change the way prosthetic limbs are thought about, developed and used.
The procedure involved numerous steps over many months:
- Les underwent targeted muscle reinnervation surgery, a procedure which reassigns nerves that once controlled the arm and hand. By reassigning the existing nerves, it became possible for Les to control his prosthetic limbs merely by thinking about the action he wanted it to perform.
- After recovery, Les was given training on the pattern recognition system that makes up a key part of the technology. Pattern recognition algorithms are used to identify individual muscles, how they are contracting, communicating and working with each other, as well as their amplitude and frequency. This information is then used to create the actual movements of the prosthesis.
- A brace was custom made for Les’s torso and shoulders. This device supports the prosthetic limbs, while also making the neurological connections with the reinnervated muscles.
- Les undertook further training on the limb system using a virtual integration environment.
- Finally, the limbs were attached to the brace, and Les was able to begin to put his training into practice, moving various objects.
Researchers were surprised by the speed at which Les was able to control the technology, particularly his ability to control a range of motions across both arms at the same time—a first for simultaneous bimanual control.
I think we are just getting started ... There is just a tremendous amount of potential ahead of us, and we've just started down this road. And I think the next five to 10 years are going to bring phenomenal advancement.Revolutionizing Prosthetics Principal Investigator, Michael McLoughlin
There was also an unexpected effect in some patients undergoing this procedure: not only can they move their new limb, they can feel some sensation with it.
Implanted myoelectric sensor technology
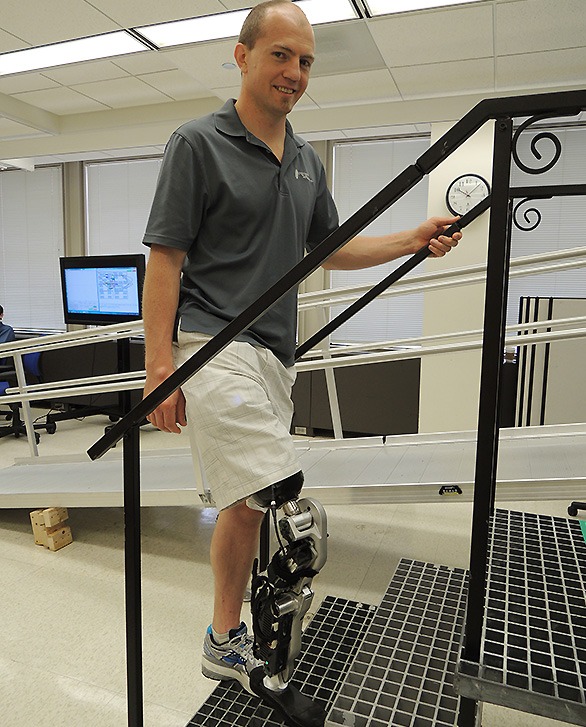
Arms aren’t the only part of the body to benefit from improved technologies. Researchers from Iceland have created a mind‐controlled prosthetic leg that uses implanted myoelectric sensor (IMES) technology. This involves sensors implanted directly into the patient’s limb muscles but, unlike nerve reinnervation, there is no need to transplant nerve tissue from one part of the body to another. Implanting the IMES technology is relatively easy and simple—requiring only a 15-minute operation where each sensor is placed into the tissue via incisions just 1 centimetre long. Once inserted, the sensors don’t need to be replaced unless they become damaged.
Thorvaldur Ingvarsson, the surgeon who completed the operation, described the process: “The technology allows the user’s experience with their prosthesis to become more intuitive and integrative ... They no longer need to think about their movements because their unconscious reflexes are automatically converted into myoelectric impulses that control their bionic prosthesis.”
A participant in the study, Gudmundur Olafsson, said, ‘As soon as I put my foot on, it took me about 10 minutes to get control of it. I could stand up and just walk away ... It was like, I was moving it with my muscles, there was nobody else doing it, the foot was not doing it, I was doing it, so it was really strange and overwhelming.’
The exciting thing about IMES technology is that it can be relatively simple to fit (it does not require complex surgery), functions well in ‘real life’ scenarios and can work for an extended period of time.
Taking this a step further, in 2015 researchers at the US Defense Advanced Research Projects Agency (DARPA) announced that they had given a paralysed man the ability to feel physical sensations via a prosthetic robotic hand that had wires directly connected to his brain. When blindfolded, the man was able to successfully identify when which fingers on his prosthetic hand were being touched, and when.
We’ve completed the circuit ... Prosthetic limbs that can be controlled by thoughts are showing great promise, but without feedback from signals travelling back to the brain it can be difficult to achieve the level of control needed to perform precise movements. By wiring a sense of touch from a mechanical hand directly into the brain, this work shows the potential for seamless bio‐technological restoration of near‐natural function.DARPA program manager, Justin Sanchez
How does it all work? An array of electrodes were clinically implanted onto the man’s sensory cortex—the region of the brain responsible for identifying tactile sensations such as pressure and texture. The team also placed arrays on the volunteer’s motor cortex, the part of the brain that directs body movements. Wires from these arrays were connected externally to a mechanical hand, which gave the volunteer the ability to control the hand’s movements. Most importantly, however, the hand contained complex torque sensors which were able to detect different levels of pressure, converting those sensations into electrical signals. These signals were then routed back to the arrays on the volunteer’s brain, stimulating the sensory neurons in the brain and allowing the sensation and feeling of each finger to be ‘felt’ by the patient.
The technology is not yet commercially available, but offers great potential for future developments.
Such advances have made these artificial limbs more practical and intuitive, but even the most state‐of‐the-art prostheses cannot yet replicate the full functionality of natural limbs.
Cosmetic improvements
The emergence of 3D printing and computer‐aided design is beginning to help create limbs that are a perfect custom‐fit for the wearer, and should, as time progresses, become more affordable.
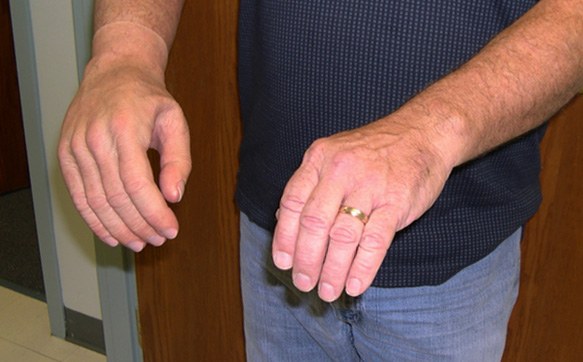
While many of the new bionics look like something out of a science‐fiction movie, researchers are also succeeding at creating options that look more realistic than ever before. Prostheses can now be created with anatomically correct shapes that mirror the form of the wearer, and can incorporate details such as accurate skin colour, freckles, birthmarks, hair, veins, tattoos, fingerprints and fingernails. These life-like creations can be made from PVC or a range of silicones and cover the prosthetic limb using a variety of methods, such as adhesive, stretchable skins, suction, form fitting, or a skin sleeve. For many amputees, having a limb that does not attract unwanted attention is very important.
Conclusion
What makes us human? Is it our bodies? Our brains? Our emotions? Or something more intangible? Advances in human bionics may eventually require us to rethink our concepts of what it is to be human, as the lines between human and machine become increasingly blurred.
Yet despite the desire to imagine a future of cybernetic enhancements, at present bionic limbs remain chiefly medical devices, designed to restore function and provide people who have lost limbs with a better quality of life. The bionics may look impressively futuristic, but they are not yet able to fully replicate the complexity, range of movement and functionality of a normal human limb.






